Why Your Veins Matter More Than You Think
Your veins silently return blood to your heart against gravity every day. Blood can accumulate in the lower legs when the one-way valves fail, triggering a series of progressively increasing symptoms. Early detection of the narrative is crucial. If any of these indications sound similar, obtain a professional inspection.
1. Heavy, Lead-Like Legs by Day’s End
That dragging, “cement-boot” feeling isn’t just fatigue. It can be an early signal of chronic venous insufficiency, where weakened valves make the return trip to your heart harder than it should be.
2. Ankles and Feet That Puff Up Without a Reason
Persistent swelling—especially if it appears most evenings or after long periods on your feet—often points to blood pooling in the lower legs. When fluid escapes into surrounding tissue, ankles and feet can look and feel puffy.
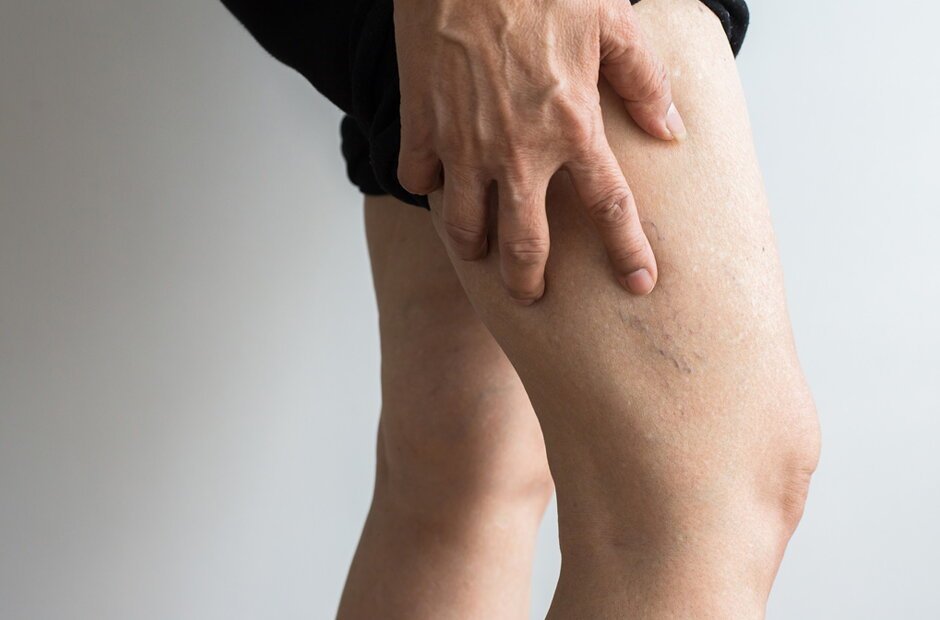
3. Ropy, Bulging Veins That Steal the Spotlight
Varicose veins aren’t just a cosmetic hiccup. Those twisted, raised cords may itch, ache, throb, or burn, and over time can increase the risk of inflammation or clots in the superficial veins.
4. Aching That Flares After Sitting or Standing
Veins thrive on movement. If your legs ache, cramp, or feel tight after hours at a desk or on your feet, your venous system may be struggling to keep blood moving in one direction.
5. Shadowy Skin Changes Around the Ankles
Reddish-brown patches, a bruise-like stain, or shiny, tight skin near the ankles can signal venous stasis—leakage of red blood cells into the skin that leaves iron deposits behind. It’s a sign to intervene before skin breaks down.
6. Itching, Dryness, or Scales That Don’t Fade
When circulation falters, skin takes the hit. Venous stasis dermatitis can look like stubborn dry skin that won’t respond to moisturizers and may be accompanied by itching, flaking, or a rash-like irritation.
7. Nighttime Cramps and Restless Legs
If your calves seize or your legs can’t stay still after dark, impaired venous return might be part of the picture. Swollen veins and low-grade inflammation can irritate tissues and nerves, sparking those after-hours disruptions.
8. Slow-Healing Sores Near the Shins or Ankles
Ulcers that linger for weeks—or keep coming back—often ride on the back of poor venous flow. Treating the wound without addressing the underlying vein problem is like mopping up with the faucet still running.
9. Warmth, Tenderness, or a Painful Line Along a Vein
A hot, tender streak that traces a visible vein can indicate superficial thrombophlebitis (vein inflammation) or a small clot. If pain and swelling are deeper, sudden, or one-sided, it could signal a more serious clot that needs urgent evaluation.
10. A Family Tree Full of Vein Troubles
Genetics set the stage. If parents or siblings have varicose veins, venous insufficiency, or a history of clots, your risk rises, even if you’re not noticing symptoms yet.
What a Vein Specialist Can Do
Modern vein consults are more didactic than mysterious. A specialist can map your circulation in real time using a targeted assessment and a painless duplex ultrasound to detect damaged valves, refluxing veins, and clots. Compression, movement breaks, elevation, and skin care are common conservative treatments. Modern techniques are minimally invasive and designed for speedy recovery.
- Sclerotherapy seals off small varicose and spider veins through tiny injections.
- Endovenous thermal ablation (laser or radiofrequency) closes problem veins from the inside, rerouting flow to healthier channels.
- Medical adhesives can shut a vein with a pinpoint application and minimal downtime.
- Microphlebectomy removes bulging tributaries through pinprick incisions.
These therapies are typically done in-office, with local anesthetic, and little to no interruption of your routine. The goal isn’t just comfort—it’s restoring efficient circulation and protecting your skin and soft tissues over the long term.
How to Read Your Body’s Clues
Vein issues tend to escalate in chapters. Early on, it’s fatigue or mild ankle swelling after a long day. Later, texture and color changes show up at the ankles. Left alone, the plot can culminate in sores, infections, or significant pain. You don’t need to wait for a dramatic twist to get answers. A short visit can tell you if what you’re experiencing is vein-related and which path forward fits your life.
Everyday Habits That Help (While You Get Checked)
While evaluation is key, simple habits can support circulation in the meantime. Mix in short walking breaks during long stretches of sitting or standing. Elevate your legs when you can. Stay well-hydrated. If recommended by a professional, wear properly fitted compression stockings. Think of these as supporting actors—not substitutes for a proper diagnosis.
When “Just Cosmetic” Isn’t
It’s easy to write off visible veins as a vanity problem, but your body is communicating. Pain, itching, swelling, skin changes, or slow-healing wounds are medical flags, not just aesthetic notes. Addressing vein health can dial down discomfort, improve sleep, and help you move with more ease, while also preventing complications you can’t see from the surface.
FAQ
What causes varicose veins?
Varicose veins usually stem from weakened vein valves that let blood flow backward and pool in the legs. Genetics, pregnancy, prolonged standing, and aging all raise the risk.
Are vein treatments painful?
Most modern vein treatments use local anesthesia and feel more like pressure or warmth than pain. Many people return to normal activities the same or next day.
Can spider veins turn into varicose veins?
They’re related but not the same; spider veins are tiny surface vessels, while varicose veins are larger and bulging. Having spider veins may signal a tendency toward venous issues but doesn’t guarantee varicose veins.
When should I worry about a blood clot?
Seek urgent care for sudden one-sided leg swelling, warmth, redness, and deep aching, especially with shortness of breath or chest pain. These can indicate a deep vein thrombosis or pulmonary embolism.
Will insurance cover vein treatment?
If symptoms affect health—like pain, swelling, ulcers, or skin changes—coverage is often possible. Purely cosmetic treatments are less likely to be covered.
Do compression stockings really work?
When properly fitted, compression supports venous return and can reduce swelling and discomfort. They’re most effective as part of a broader treatment plan.
Can exercise make varicose veins worse?
Low-impact movement like walking, cycling, and swimming generally helps circulation. Heavy straining without proper breathing technique can temporarily worsen bulging veins.
How long do results from vein procedures last?
Treated veins typically stay closed permanently, but new problem veins can appear over time. Regular follow-ups and supportive habits help maintain results.
Is surgery still common for varicose veins?
Open surgery is far less common today. Minimally invasive procedures have largely replaced it for many cases, with excellent outcomes and faster recovery.
Do men get varicose veins too?
Yes—vein disease affects all genders, though it’s often underreported in men. The signs and treatments are similar for everyone.